The carotid arteries are major blood vessels that branch out from the aorta, the largest artery in the body, and transport oxygen-rich blood to the brain and are located on the left and right side of the neck.
Carotid artery disease refers to the obstruction of one or both arteries, decreasing blood flow to the brain. In severe blockage and when diseased, this could lead to a stroke. Carotid artery disease develops slowly, and a stroke or transient ischemic attack (TIA) may be the first indication that you have the disease. TIAs start suddenly, and they resolve reasonably quickly as well. A typical TIA lasts only minutes, and in less than one hour, half of all patients feel relatively normal. The longer the symptoms continue, the less likely they are to resolve on their own; by definition, they are not due to TIAs, but strokes, with symptoms that last for more than 24 hours.
According to the CDC, 795,000 Americans have a stroke every year. The vast majority of these cases are the result of atrial fibrillation or carotid artery disease and is responsible for over half of all stroke cases in the United States.
What Causes Carotid Artery Disease?
Like myocardial infarction (i.e., heart attack), carotid artery disease occurs when plaque builds up in the carotid artery, obstructing the normal blood flow.
Atherosclerotic Plaque Contains:
Cholesterol
Fat
Protein
Calcium
Cellular waste
When the plaque accumulates enough, the carotid artery becomes narrower, and the amount of blood reaching the brain drops.
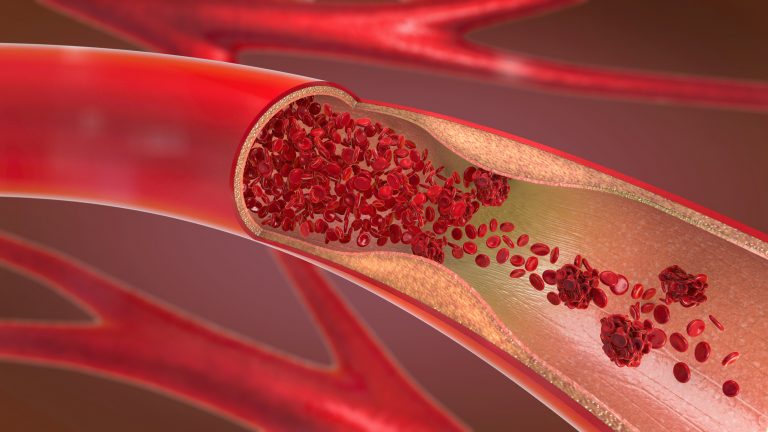
Risk Factors:
Advanced age – arterial walls are composed of endothelial cells, which accumulate damage as we age
Chronic blood hypertension – the high pressure inside the blood vessels damage the artery, which increases the risk of atherosclerosis
High cholesterol levels – oxidized LDL (i.e., bad cholesterol) is the main form found in atherosclerotic arteries
Diabetes – similar to hypertension, high blood glucose is damaging for the arterial walls
Obesity – researchers identified obesity as an independent risk factor of carotid artery disease
Sedentary lifestyle – physical inactivity increases the risk of diabetes, chronic hypertension, and obesity
Smoking – cigarette smoke contains hundreds of harmful chemicals that irritate arteries and precipitate carotid artery disease
Family history – having a family history of coronary artery disease, strokes, or peripheral artery disease increases your risk of developing atherosclerosis
The Signs and Symptoms of Coronary Artery Disease:
Generally speaking, carotid artery disease does not cause any symptoms. Once the arteries become narrowed enough, only then do symptoms arise.
When the artery becomes narrow, you could develop a transient ischemic attack (TIA) or a stroke. Depending on the specific area affected by blood deprivation, you can expect different signs and symptoms of a stroke. Additionally, the faster patients are provided with the proper care, the better their outcome will be.
The Most Common Signs and Symptoms of Stroke:
Paralysis
Unilateral (i.e., one-sided) numbness or weakness (e.g., arm, face, leg)
Trouble speaking or understanding speech
Confusion
Slurring speech
Vision problems (e.g., double vision, blurred vision)
Trouble walking
Loss of balance or coordination
Dizziness
Severe headache
How Carotid Artery Disease is Diagnosed:
To make the diagnosis of carotid artery disease, your doctor will take your medical and family history, followed by a comprehensive physical examination. However, the definitive diagnosis of carotid artery disease is confirmed by imaging tests.
Diagnostic Tests for Carotid Artery Disease:
Carotid Ultrasound is a noninvasive test that uses sound waves to measure the flow and blood pressure in the carotid arteries. Ultrasound can also estimate the degree of narrowing.
Computed Tomography Angiography is an advanced imaging technique that is a type of x-ray combined with a contrast (i.e., a dye that “lights up” the studied blood vessels and tissues) to take detailed pictures of the carotid arteries.
Magnetic Resonance Angiography uses contrast to highlight the blood vessels of the neck and brain, and a 3D image is taken to locate the site of vessel obstruction accurately.
Treatment Options:
The treatment of the disease highly depends on whether you’ve had a prior stroke or not. If your doctor makes the diagnosis of carotid artery disease before having a transient ischemic stroke, he/she will suggest lifestyle modifications to prevent this complication.
These include:
Exercising regularly
Eating healthy food
Quitting smoking
Managing chronic conditions (e.g., heart disease, diabetes, atrial fibrillation)
Taking medications that lower the risk of stroke (e.g., aspirin, statins)
If the patient develops a stroke and carotid artery disease is the culprit, the treatment becomes more invasive.
The Primary Methods to Remove Carotid Artery Obstruction:
Carotid Endarterectomy is the most common form of surgery performed for severe carotid artery disease cases. After undergoing general anesthesia, your doctor will make an incision on your neck, which gives him/her access to the carotid artery to remove the plaque.
Carotid Angioplasty and Stenting is the other option to remove the obstruction in your carotid artery. Your doctor will insert a stent (i.e., a small wire coil) to keep the artery open. Angioplasty enlarges the region so that blood can circulate freely; the operation involves briefly inserting and inflating a tiny balloon into the clogged artery.
Opting for a carotid artery stent is reasonable in the following cases:
The location of the blockage is inconvenient
The blockage is substantial
You have other concurrent medical conditions that contraindicate surgery
Before choosing any treatment, you will have detailed discussions with your doctor about the best option for your case, as well as the safety, effectiveness, and potential complications of each procedure.